Patient information about Ankle Stabilisation Surgery
This page provides general information for patients of Dr. Borshch in Brisbane, who are preparing for Orthopaedic ankle stabilisation surgery for chronic ankle instability.
Your individual condition and treatment plan may be different, so this information should be used alongside the advice of your surgeon and treating team.
What is it?
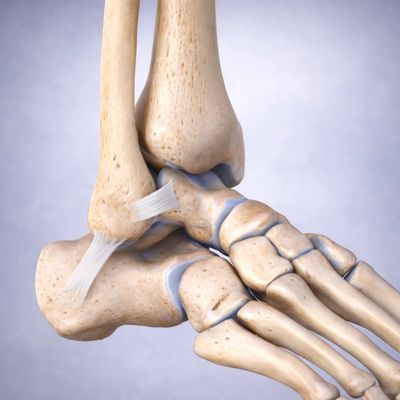
The ankle is stabilised by several ligaments. The most commonly injured are the lateral ankle ligaments on the outside of the ankle, especially:
- ATFL (anterior talofibular ligament)
- CFL (calcaneofibular ligament)
After a significant ankle sprain, these ligaments can heal stretched or weak. This can lead to chronic lateral ankle instability—the ankle repeatedly “rolls”, feels unreliable, or gives way.
Ankle stabilisation surgery (often called lateral ankle ligament repair or reconstruction) aims to:
- improve ankle stability
- reduce repeated sprains
- reduce pain and swelling
- help return safely to work, sport, and day-to-day activity
Why is it done?
Most ankle sprains improve with rehabilitation, especially strength and balance training. Surgery is usually considered when there is ongoing instability despite appropriate non-surgical treatment.
Common reasons include:
- repeated ankle sprains (especially on uneven ground or with sport)
- ongoing “giving way” episodes
- persistent pain/swelling and reduced confidence
- failure of physiotherapy, bracing, and activity modification
- high physical demands (sport, physical work)
Chronic ankle instability is also associated with cartilage damage and may contribute to longer-term joint wear if the instability persists. (https://pubmed.ncbi.nlm.nih.gov/19122084/)

How is it done?
Exact details vary, but most ankle stabilisation operations involve:
Anaesthetic
- Usually a general anaesthetic, often combined with local anaesthetic around the ankle for pain control.
Assessing the ankle
- Some cases are done with arthroscopic assistance (keyhole camera) to check for cartilage injury, scar tissue, or loose fragments in the ankle joint, and to treat these if needed.
Ligament repair (commonly a Broström-type repair)
- The damaged ligaments are tightened and reattached to bone (often using small anchors).
- This is a common operation for chronic lateral ankle instability and is supported by guideline-based recommendations. (https://pubmed.ncbi.nlm.nih.gov/31579683/)
Augmentation or reconstruction (only if needed)
- If the ligaments are too damaged, or the ankle is very unstable, the repair may be augmented (reinforced) or reconstructed using a graft/strong internal support.
- Randomised/prospective studies suggest augmentation techniques can allow earlier return to activity in selected patients (without clearly higher complication rates in those studies). (https://pubmed.ncbi.nlm.nih.gov/33491480/)
Closing the incision
- The wound is closed with sutures and dressings.
- A splint/boot is used to protect the repair while it heals.
- Arthroscopic (keyhole) and open approaches are both used; evidence suggests similar overall outcomes in many patients, with technique chosen based on anatomy, surgeon preference, and the exact problem being treated. (https://pubmed.ncbi.nlm.nih.gov/37964306/)

How to prepare for surgery.
Good preparation lowers risk and helps recovery.
Health optimisation (very important)
- Stop smoking/vaping if possible (smoking increases wound-healing problems).
- If you have diabetes, aim for good blood sugar control.
- Tell the team about any history of blood clots, heart/lung disease, or immune-suppressing medications.
Prehab (exercise before surgery)
Physiotherapy before surgery is valuable and usually focuses on:
- calf strength
- balance/proprioception
- hip and core control
- swelling reduction and maintaining ankle movement
Home preparation
- Arrange help for the first 1–2 weeks (shopping, school runs, meals).
- Prepare for a period of reduced mobility: clear trip hazards and plan safe paths at home.
- Set up leg elevation and icing options.
Medications
Your team will advise what to stop or continue (for example, blood thinners, anti-inflammatories, or supplements). Always check before changing anything.
What to expect after surgery.
In hospital (usually overnight surgery)
- Pain control using a multimodal plan.
- You go home in a boot or splint, usually with crutches.
- You will be given a plan for wound care and follow-up.
First 2–6 weeks
- Often protected weight-bearing in a boot (exact timing depends on the procedure).
- Swelling is common (often worse later in the day).
- Physiotherapy usually begins with safe movement, swelling control, and gentle activation exercises.
6 weeks to 3 months
- Transition from boot to normal footwear as advised.
- Progressive strengthening and balance work.
- Walking and daily activities improve steadily.
3 to 12 months
- Higher-level balance, agility, and sport-specific training.
- Return to sport is guided by strength, balance, control, and confidence (timing varies by the operation and your goals).
Long term outcomes.
Stability and function
Most patients have good to excellent improvement in stability and function after surgery for chronic lateral ankle instability. Meta-analyses comparing surgical techniques support generally strong outcomes, with procedure choice based on the individual situation. (https://pubmed.ncbi.nlm.nih.gov/29940985/)
Joint protection
Ongoing instability is associated with cartilage injury and early joint changes in some studies. Stabilising the ankle may help reduce repeated injury and abnormal joint loading. (https://pubmed.ncbi.nlm.nih.gov/19122084/)
Things to look out for (and when to seek help)
Things to look out for (and when to seek help)
Contact our office, your GP, or go to hospital urgently if you notice:
Possible infection
- increasing redness, warmth, or swelling around the incision
- worsening pain after initial improvement
- discharge or pus
- fevers or feeling unwell
Blood clot warning signs
- new calf pain/tenderness or increasing swelling in one leg
- sudden shortness of breath, chest pain, coughing blood (call emergency services)
Wound problems
- leaking through dressings
- opening wound edges
- rapidly increasing bruising or swelling
Nerve irritation (usually temporary)
- numbness or tingling around the foot/ankle that is worsening rather than improving
Recurrent instability
- ongoing giving way after the early recovery period
- repeated sprains despite rehabilitation

My take on Ankle Stabilisation surgery
Ankle stabilisation surgery can be very effective for people with ongoing ankle instability after repeated sprains, especially when physiotherapy and bracing have not been enough. The best outcomes come from:
- choosing surgery for the right reason (true instability, not just pain)
- addressing associated problems (cartilage injury, impingement, alignment) when present
- a structured rehabilitation plan focused on strength and balance
Copyright © 2026 Dr. Alexey Borshch - All Rights Reserved.